Aortic stenosis is one of the most common and serious valve diseases of the heart. Often progressing silently for years, it can remain unnoticed until symptoms such as chest pain, breathlessness, or fainting appear. Early detection and timely treatment are critical, as modern therapies now offer safer and less invasive options than ever before.
What is Aortic Stenosis?
Aortic stenosis definition: Aortic stenosis is a heart valve disorder where the aortic valve which is the gateway between your heart’s main pumping chamber and the aorta becomes narrowed and stiff. This narrowing restricts blood flow from the heart to the rest of your body, forcing your heart to work harder to pump blood effectively.
To understand what is stenosis, think of it as a narrowing or constriction of any passage in the body. In the case of aortic stenosis, the valve leaflets become thickened, calcified, or fused together, creating a smaller opening for blood to pass through.
It’s important to distinguish between aortic valve sclerosis and aortic stenosis. Aortic valve sclerosis represents the early stage of valve deterioration, where the valve becomes thickened and stiff but doesn’t significantly restrict blood flow. As the condition progresses, it can develop into aortic stenosis, where the narrowing becomes severe enough to impair heart function.
Aortic stenosis is a serious, progressive condition that can be life-threatening if left untreated. Without proper intervention, severe aortic stenosis can lead to heart failure, dangerous arrhythmias, and sudden cardiac death. However, with early detection and appropriate treatment, patients can maintain good quality of life and improved outcomes.
Causes of Aortic Stenosis
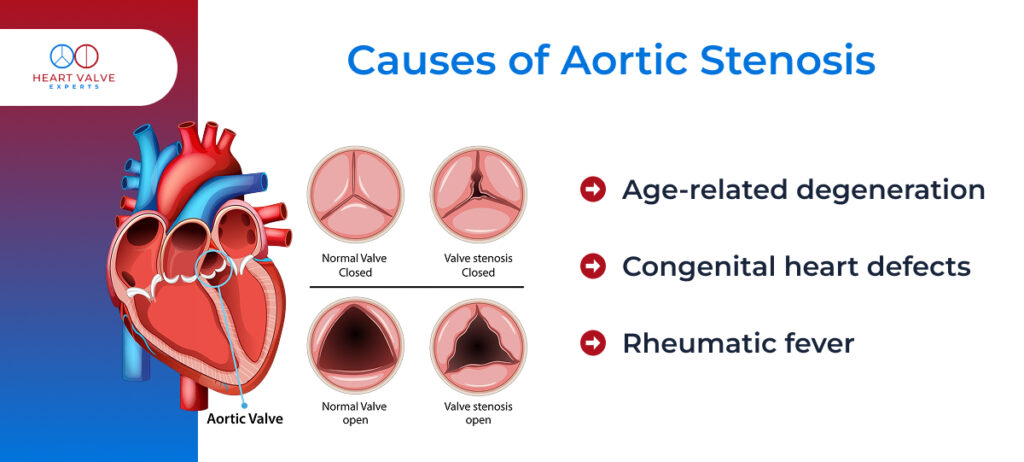
Understanding aortic stenosis causes, helps identify who might be at risk and enables early intervention. The primary aortic valve stenosis causes include:
Age-related degeneration:
The most common cause in developed countries. As we age, calcium deposits naturally accumulate on the aortic valve leaflets, causing them to stiffen and narrow. This process typically affects people over 65 years old and occurs gradually over many years.
Congenital heart defects:
This represents another significant cause, particularly bicuspid aortic valve. This is a condition where the valve has two leaflets instead of the normal three. People born with this defect often develop aortic stenosis earlier in life, typically in their 40s or 50s, because the abnormal valve structure leads to increased wear and tear.
Rheumatic fever:
Though less common in developed countries today, rheumatic fever remains a leading global cause of long-term heart valve damage. This inflammatory condition results from untreated strep throat infections and can lead to valve scarring and stenosis years later. The damage occurs when the body’s immune response to the infection mistakenly attacks heart valve tissue.
Risk Factors for Aortic Stenosis
Several aortic stenosis risk factors increase your likelihood of developing this condition. Understanding these factors can help with prevention strategies and early detection:
Advanced age:
The strongest risk factor, with most cases occurring in people over 65. The natural aging process leads to valve calcification and stiffening over time, making older adults particularly susceptible.
High blood pressure:
This puts additional strain on the aortic valve over time, accelerating wear and calcification. The increased pressure forces the valve to work harder with each heartbeat, contributing to faster deterioration.
Smoking:
Damages blood vessels and accelerates atherosclerosis, which can contribute to valve deterioration. The toxins in cigarette smoke also promote inflammation and calcium deposits throughout the cardiovascular system.
Diabetes:
Associated with increased calcium deposits on heart valves and accelerated atherosclerosis. High blood sugar levels over time can damage blood vessels and heart structures, including the aortic valve.
Family history:
Plays a role, as genetic factors can influence valve structure and susceptibility to calcification. If close relatives have had aortic stenosis, your risk may be higher.
High cholesterol levels:
This may contribute to valve calcification, similar to how they affect coronary arteries. Some research suggests that elevated cholesterol can accelerate the deposit of calcium on valve leaflets.
Aortic Stenosis Signs and Symptoms to Watch For
Aortic stenosis symptoms can be subtle initially, making early detection challenging. The condition often progresses silently for years before symptoms appear, which is why regular cardiac checkups are crucial, especially for those at higher risk.
The classic triad of aortic stenosis signs and symptoms includes:
- Chest pain or pressure often occurs during physical activity. Patients describe it as a heavy, squeezing sensation similar to angina. This happens because the narrowed valve prevents adequate blood flow to meet the heart’s increased oxygen demands during exercise.
- Shortness of breath typically begins with exertion but can progress to occur at rest. Patients may notice difficulty climbing stairs, walking distances they previously managed easily, or feeling winded during routine activities.
- Fainting or near-fainting episodes (syncope) are particularly concerning symptoms. These occur because the narrowed valve can’t deliver enough blood to the brain during periods of increased demand, such as exercise or sudden position changes.
Additional symptoms may include:
- Heart palpitations or irregular heartbeats, as the heart struggles to maintain adequate circulation through the narrowed valve.
- Fatigue and weakness that seems disproportionate to activity level, reflecting the heart’s decreased ability to pump blood efficiently.
- Swollen ankles and feet, indicating possible heart failure development.
It’s crucial to understand that early aortic stenosis signs and symptoms may be completely absent. Many patients remain asymptomatic until the stenosis becomes severe, which is why the condition is sometimes called a “silent killer.” Once symptoms develop, the condition has typically progressed significantly, making timely intervention critical.
How Aortic Stenosis is Diagnosed?
The diagnostic process typically begins when a doctor detects a heart murmur during a routine physical examination or when a patient reports concerning symptoms.
Echocardiogram:
The gold standard diagnostic tool for aortic stenosis. This non-invasive ultrasound test provides detailed images of the heart valves and measures blood flow velocity across the aortic valve. It can determine the severity of stenosis and assess heart function.
- Electrocardiogram (ECG): Records the heart’s electrical activity and may reveal signs of left ventricular hypertrophy (thickening of the heart’s main pumping chamber that occurs as it works harder against the narrowed valve).
- Chest X-ray: To show heart enlargement and signs of heart failure, though it’s less specific than other tests.
- Cardiac CT scan: Provides detailed images of the aortic valve and can help measure calcium deposits, which correlate with stenosis severity.
- Cardiac catheterization: Performed in some cases to directly measure pressures across the valve and assess coronary arteries before potential surgery.
- Exercise stress testing: Conducted in asymptomatic patients to evaluate how the heart responds to increased demands and identify subtle symptoms that emerge with exertion.
Early detection is paramount because it allows for careful monitoring and timely intervention before complications develop. Regular follow-up appointments help track disease progression and determine optimal treatment timing.
Modern Treatment Options
Aortic stenosis cannot be cured with medication, but drugs may help manage symptoms and related conditions. Blood pressure medicines, diuretics, rhythm-control drugs, and cholesterol-lowering therapy can reduce strain on the heart and ease discomfort, yet they do not correct the narrowed valve. Definitive treatment requires valve replacement. Modern treatment options are led by groundbreaking minimally invasive approaches:
Minimally Invasive Treatments
- Transcatheter Aortic Valve Replacement (TAVR/TAVI):
TAVR has transformed the way aortic stenosis is treated. Instead of open-heart surgery, a new valve is delivered through a thin catheter, usually inserted in the groin artery, and placed inside the diseased valve without removing it.
- Advantages include:
- Shorter hospital stay (often discharged in 1–3 days).
- No need for opening the chest or using a heart-lung bypass machine.
- Safer option for elderly or high-risk patients.
- Valve-in-Valve TAVR:
For patients who previously had a biological (tissue) valve that has worn out over time, a valve-in-valve procedure can restore function without the risks of repeat open-heart surgery.
- A new transcatheter valve is positioned inside the failing surgical valve.
- Offers quicker recovery, less pain, and lower surgical risk compared to redo surgery.
- Particularly valuable for elderly patients or those not fit for another open-heart operation.
- Balloon Valvuloplasty:
In some patients, especially those who are critically ill or not yet candidates for valve replacement, balloon valvuloplasty may be used. In this procedure, a balloon catheter is inserted and inflated to stretch the narrowed valve.
- Helps in temporary symptom relief or a bridge to definitive treatment.
- Not a long-term solution as the valve usually narrows again over time.
Traditional Surgical Options
- Surgical Aortic Valve Replacement (SAVR):
SAVR remains the gold standard in many patients, particularly younger individuals or those needing additional heart surgery. In this open-heart procedure, the diseased valve is completely removed and replaced with a new one.
- Types of replacement valves:
- Mechanical valves: Very durable, but require lifelong blood thinners.
- Biological (tissue) valves: Don’t require lifelong anticoagulation but may wear out faster.
- Considerations:
- Involves cardiopulmonary bypass and longer recovery.
- Offers excellent long-term outcomes when performed in suitable patients.
Prevention and Heart Health Tips
Prevention of aortic stenosis focuses on modifiable risk factors, as age-related valve degeneration cannot be completely avoided. However, certain strategies may help slow its progression and reduce overall cardiovascular risk:
- Control cholesterol levels through diet, exercise, and medications when necessary. Some studies suggest that lowering cholesterol may slow valve calcification, though this remains an area of ongoing research.
- Quit smoking immediately, as tobacco use accelerates atherosclerosis and valve deterioration. Smoking cessation provides immediate and long-term cardiovascular benefits.
- Manage blood pressure effectively through lifestyle modifications and medications. Controlled blood pressure reduces strain on the aortic valve and entire cardiovascular system.
- Control diabetes through proper diet, exercise, and medication management. Good glycemic control reduces cardiovascular complications and may slow valve deterioration.
- Maintain a heart-healthy diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats. Limit processed foods, excessive salt, and saturated fats.
- Exercise regularly as appropriate for your condition. While people with severe aortic stenosis may need activity restrictions, most patients with mild to moderate stenosis benefit from regular, moderate exercise.
- Regular heart screenings are essential, especially for those with risk factors or family history. Early detection allows for proper monitoring and timely intervention.
Conclusion: Advanced Care for Aortic Stenosis
Aortic stenosis is a serious but treatable condition when properly diagnosed and managed. The landscape of treatment has been revolutionized by minimally invasive procedures like TAVR, offering hope to patients with faster recovery times and excellent results.
If you’re experiencing symptoms like chest pain, shortness of breath, or fainting episodes, don’t delay seeking medical evaluation. Our team specializes in minimally invasive procedures for aortic stenosis and is committed to providing personalized care that considers your unique situation and treatment goals.
Take the first step toward better heart health. Schedule your consultation with our expert heart valve specialists today and explore the most advanced, minimally invasive treatment options designed to restore your quality of life. Visit Heart Valve Experts to connect with our team and get personalized guidance for your heart.
FAQs:
No. Medicines only ease symptoms. Definitive aortic stenosis treatment requires valve replacement.
It can stay stable for years. Once aortic stenosis symptoms appear, it often worsens quickly.
Mainly through echocardiography, which confirms the aortic stenosis presence and severity.
Without treatment, survival is often 2 to 5 years for patients with severe symptomatic AS. Valve replacement greatly improves outcomes.
You cannot fully prevent it, but managing aortic stenosis risk factors like high BP, cholesterol, and smoking may slow progression.